H P Template Pdf - History and Physical Examination H P Examples The links below are to actual H Ps written by UNC students during their inpatient clerkship rotations The students have granted permission to have these H Ps posted on the website as examples
required physical exam elements for h p required exam elements for all sedation without an anesthesiologist present denotes extra caution required eyes wnl abnormal gu wnl abnormal ent wnl abnormal gyn wnl abnormal cardiac wnl
H P Template Pdf

H P Template Pdf
Example of a Complete History and Physical Write-up Patient Name: Unit No: Location: Informant: patient, who is reliable, and old CPMC chart. Chief Complaint: This is the 3rd CPMC admission for this 83 year old woman with a long history of hypertension who presented with the chief complaint of substernal “toothache like” chest pain of 12 hours
2 Dyspnea final written H P and just list a final problem list 3 History of HTN 4 years shown below it is useful to make an initial list simply 4 History of TAH BSO to keep track of all problems uncovered in the interview 5 History of peptic ulcer disease 1 9 in this list and exam 10 13 6 Penicillin allergy 7
HISTORY Amp PHYSICAL SHORT FORM PROCEDURE UCLA
Comprehensive Adult History and Physical Sample Summative H P by M2 Student This sample summative H P was written by a second year medical student from UCF COM Class of 2020 at the end of COP 2 While not perfect it best exemplifies the documentation skills students are expected and able to acquire by the end of P 2 organization

H P Template Pdf Fill Online Printable Fillable Blank PdfFiller
Template for Dictating a History and Physical Ext 2 9007 work type 09 Enter FIN not MRN State your name Patient Name Patient MRN and FIN Admitting Attending Date of service Date Patient Name Patient MR FIN General Appearance Chief Complaint PCP Reason for Admission Code Status Surrogate Decision Maker

Printable Blank H P Template

History And Physical Template Fill Online Printable Regarding
History And Physical Examination H Amp P Examples
The written History and Physical H P serves several purposes It is an important reference document that provides concise information about a patient s history and exam findings at the time of admission It outlines a plan for addressing the issues which prompted the hospitalization
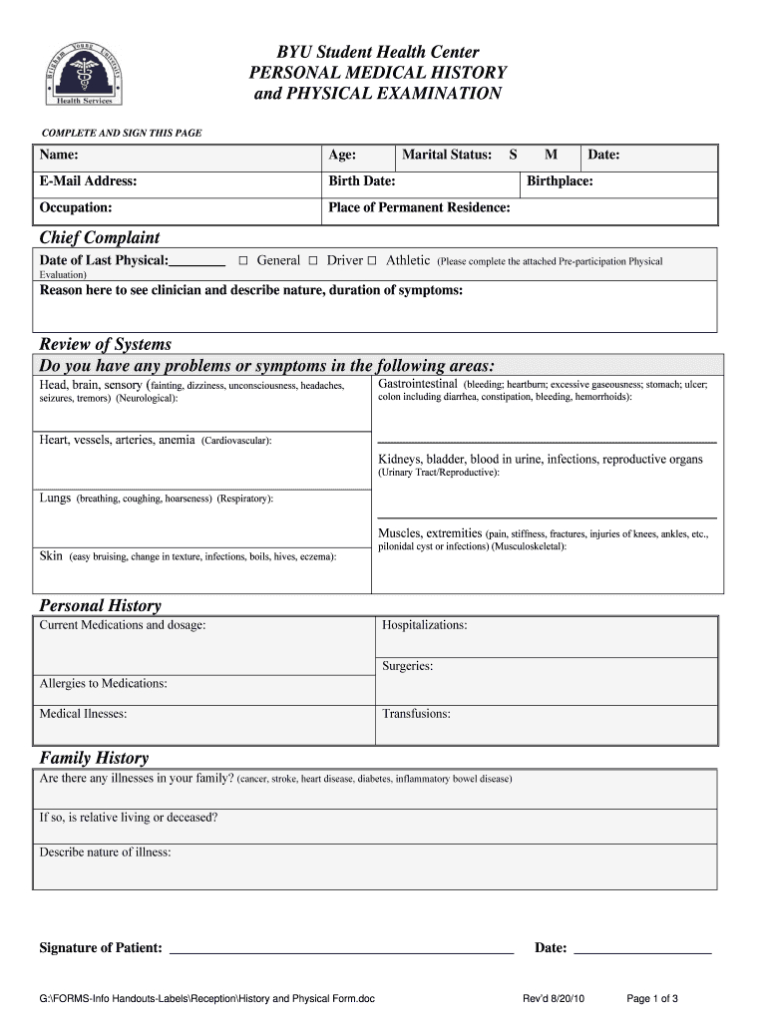

H P Template Fill Online Printable Fillable Blank Regarding
History and Physical Evaluation Form Please fax completed form to 302 777 2111 Patient Name Age Gender Pre Op Diagnosis Proposed Surgery
History And Physical Form PDF Details. Physicians have been using the history and physical form (H&P) for years to help them diagnose their patients. The form is a summary of a patient's medical history and current condition, which can help physicians identify potential problems early on.
Example Of A Complete History And Physical Write Up
General Guidelines formatmay vary atdifferentsites emphasis may change fordifferentpatients Psychiatry H P I D name age gender housing marital status

H P Template Fill Online Printable Fillable Blank Throughout

History And Physical Template Fill Online Printable Regarding
H P Template Pdf
History and Physical Evaluation Form Please fax completed form to 302 777 2111 Patient Name Age Gender Pre Op Diagnosis Proposed Surgery
required physical exam elements for h p required exam elements for all sedation without an anesthesiologist present denotes extra caution required eyes wnl abnormal gu wnl abnormal ent wnl abnormal gyn wnl abnormal cardiac wnl

Printable H p Template Printable Word Searches

Printable H p Template Printable World Holiday
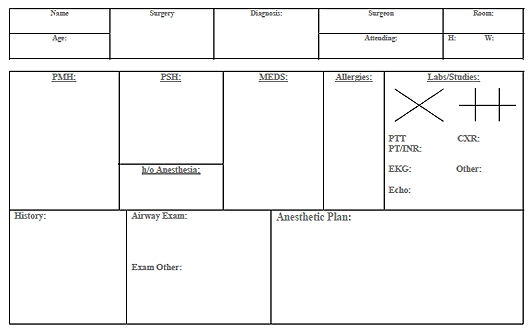
Pediatric H p Template

Patient Interview Template PDF Instant Digital Download Etsy

Psychiatry H P Clinical Template For Medical Students And Etsy Norway